 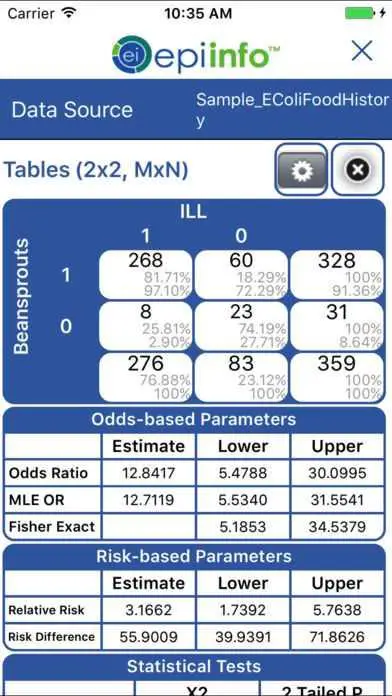
avium complex) the radiologic manifestation was infiltrate in 54% of patients and less than 10% had bronchiectasis or a cavity. In a recent study of patients with lung disease due to NTM (90% M. Radiologic manifestations sometimes included infiltrates, consolidation or masses – rather then the NB or FC features specified in the definitions. In some cases only a single sputum sample could be obtained and in other cases only one of multiple specimens was positive. #Epi info 72 download for mac for mac#In many cases only a single expectorated sputum was positive for MAC in a patient with pulmonary symptoms, but treatment was compelled by symptoms, radiologic evidence of a new pulmonary process, and no alternate diagnosis. Missing criteria fell into two major categories: microbiologic and radiologic. This review of 13 years' experience with the treatment of MAC pulmonary disease at an academic medical center indicates that a substantial proportion of patients deemed by pulmonary or infectious disease specialists to require treatment do not meet current ATS/IDSA criteria for MAC pulmonary disease. If patients were noted to have bronchiectasis for the first time at the time of MAC diagnosis, they were classified as primary, whereas if they had a diagnosis of bronchiectasis prior to their MAC diagnosis they were classified as having secondary disease. Patients with unknown smoking history or non-pulmonary co-morbidities (e.g., Behcet's disease, rheumatoid arthritis) were classified as having primary disease. Patients with known history of smoking were also classified as secondary. Secondary disease was defined as disease occurring in a patient with known antecedent lung disease at time of MAC diagnosis such chronic obstructive pulmonary disease, asthma, or pre-existing bronchiectasis. Primary disease was defined as disease occurring in persons without known antecedent pulmonary disease at time of MAC diagnosis. We classified MAC pulmonary disease as primary or secondary. We determined whether cases met American Thoracic Society/Infectious Disease Society of America (ATS/IDSA) diagnostic criteria for MAC pulmonary disease ( Table 1) and whether they had findings of fibrocavitary or nodular/bronchiectatic disease by radiography. All imaging interpretations were abstracted from the official radiology report. If a patient had both chest CT scan and chest x-rays performed, CT scan results were used preferentially over x-ray results to classify patients. For each patient, we abstracted demographic, clinical, radiologic, and laboratory data, past and current treatment details, adverse drug reactions, and outcomes data from the medical record. Patients were included if they had MAC pulmonary disease and were either referred to the medical center after diagnosis or were diagnosed at the medical center. #Epi info 72 download for mac code#We identified patients using the International Statistical Classification of Diseases (ICD-9) code for MAC. We performed medical record review of both electronic and paper records for all HIV-negative patients aged >18 years who were diagnosed with Mycobacterium avium complex (MAC) pulmonary disease from 1993 through 2006 and were treated by pulmonary (n = 20), infectious disease (n = 42), or both (n = 10) specialists at an academic medical center. Based on our experience we propose that a larger prospective study be conducted using expanded definitions for epidemiologic and clinical studies with a new dichotomous system for classifying cases based on the presence or absence of underlying lung disease at the time of MAC diagnosis. We report on all treated patients, including those who did not meet ATS/IDSA definitions. In the present report, we summarize our 13-year experience in the diagnosis and treatment of MAC pulmonary disease at an academic medical center. Further, contemporary imaging studies often disclosed features of both FC and NB disease, or other manifestations, making dichotomous radiologic categorization difficult. Our experience at an academic medical center suggested that a significant proportion of patients determined by infectious disease or pulmonary specialists to require treatment for MAC pulmonary disease did not meet ATS/IDSA microbiologic criteria. #Epi info 72 download for mac full#Many published studies of pulmonary MAC exclude a substantial number of patients who do not meet full ATS/IDSA criteria.  
ATS/IDSA criteria for the diagnosis of non-tuberculous mycobacterial lung disease. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
